CCHR warns of treatments (electroshock, antidepressants) that can induce, not prevent suicide
By Jan Eastgate
President, CCHR International
The Mental Health Industry Watchdog
Anesthetics that induce unconsciousness and a loss of sensation and awareness are being used as experimental drugs to treat depression. This includes an anesthetic also known as a “date rape” drug and a recent depression study using propofol—the anesthetic that killed Michael Jackson.[1] People in need of help are being consistently put at risk by the treatments the Food and Drug Administration (FDA) has approved and by researchers and practitioners in the mental health system recommending them, including antidepressants and electroshock. The misleading information given consumers should be investigated, especially when marketed as being prescribed for “treatment resistance,” a term invented to explain away treatment failure.
The FDA that approves these drugs needs an overhaul. CCHR has documented a list of some 36 FDA-approved drugs since the 1970s that were recalled due to adverse reactions. Of these, five were psychiatric drugs. Fourteen drugs have been linked to more than 58,300 deaths. That doesn’t include the psychotropic drugs approved that have potential tens of thousands of deaths and serious adverse events linked to them but remain on the market.
Jackson died 10 years ago, receiving a lethal dose of propofol that his doctor, Conrad Murray prescribed for insomnia. Murray was convicted of involuntary manslaughter in 2011. [2] Jackson was given a 25mg propofol injection.[3]
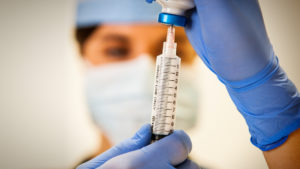
In the depression study, patients received up to about 12 mgs of propofol intravenously. Only 10 subjects were used to claim “success,” measured by half having maintained “better moods for three months.” In other words, the other half failed to experience this and none were cured.
In the depression study, patients received up to about 12 mgs of propofol intravenously. Only 10 subjects were used to claim “success,” measured by half having maintained “better moods for three months.” In other words, the other half failed to experience this and none were cured.[4] The researchers do not know how propofol supposedly “works” for depression, but theorize it “may be triggering the brain to reorganize itself” or “coaxing the brain into getting unstuck from this bad, depressed state that it’s in.”[5]
We’ve heard of similar, unproven theories in relation to antidepressants and electroshock treatment. Most recently The Wall Street Journal claimed that 460 volts of electricity sent searing through the brain may help to “realign disrupted circuits.”
However, depression, bipolar—in fact, all mental disorders—cannot be physically identified in the brain, not even at autopsy. Propofol is claimed to have fewer side effects than brain stimulation interventions such as electroshock, which has side effects that include “confusion and memory loss,” according to an ABC news affiliate article about the study.[6] ECT also may also cause brain damage and death.
The FDA and American Psychiatric Association (APA) claim the merits of electroshock over antidepressants and other mind-altering drugs, although there are no clinical trials proving ECT’s safety and efficacy. And serious risks are often minimized.
ECT proponent, Charles Kellner, professor of psychiatry at Icahn School of Medicine at Mount Sinai and director of its ECT service recently asserted in Psychiatric Times that adverse effects such as the cognitive damage that ECT causes shouldn’t be seen as a “safety” concern but, rather, a “tolerability” issue. He argued that “safety” means risk of “physical injury,” and “To elevate cognitive adverse effects to this level perpetuates the stigma surrounding ECT.” Astoundingly he claims that “refusing ECT because of concerns about memory loss is equivalent to refusing cancer chemotherapy because of concerns about hair loss.” And, as with chemotherapy, “most of the hair grows back;” similarly, with ECT, “most of the memories return.”
There is no comparison. There are no tests or imaging scans that can confirm a diagnosis of depression physically existing in the brain or elsewhere in the body. But tests do exist to confirm cancer, which can be found in cell or tissue samples under a microscope and shown by imaging tests. Chemotherapy can prevent cancer cells from growing and spreading by destroying the cells or stopping them from dividing. Antidepressants and electroshock do not and cannot prevent “depression cells” from growing or spreading because they don’t exist.
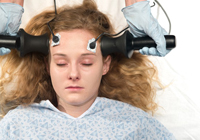
ECT is not “life-saving” and is not proven to clinically prevent suicide. In fact, it can induce suicide.
ECT is not “life-saving” and is not proven to clinically prevent suicide. In fact, it can induce suicide. For example:
- A coroner’s inquest in Australia determined that involuntary ECT did not prevent but may have led to a patient’s death after a suicide attempt.[7]
- A UK coroner investigating the death of mother of one, Katherine Rought-Rought in June 2016 found that the ECT she’d been administered had led to a “deterioration in her mental health…culminating in her decision to commit suicide.”[8]
- Researchers reviewed more than 90 ECT studies since 2010 and found: “There is still no evidence that ECT is more effective than placebo for depression reduction or suicide prevention.”[9]
Few consumers are told of the suicidal risks from both ECT and antidepressants. Dr. Michael Hengartner, of Zurich University in Switzerland, who led a recent study on antidepressants stated, “We can be confident that these drugs are producing an excess rate of suicides, beyond the depression itself. There is no doubt that this must be a response to the pharmacological effect of the drugs themselves.”[10]
The history of the approval and use of dangerous treatments for those labeled mentally disordered is one of abject failure. And that is marketed not as failure, but as the patient’s “resistance” to treatment!
Even Dr. Allen Francis, former head of the APA’s fourth edition of its Diagnostic & Statistical Manual of Mental Disorders (DSM), admitted: “We use terms like treatment-resistance and treatment-refractory, but this is merely an admission of our failure to have a solution.” Further, “We persist in treatment, usually by giving whatever has failed previously in more dosage or by adding new treatments that have little chance of success, but a high risk of side effects.”[11]
As an example, the FDA recently approved an anesthetic nasal spray, esketamine (Spravato) as an adjunct to antidepressants for treatment of depression, despite the fact it has not been scientifically proven to reduce the risk of suicide.[12] There was only one “successful” short-term, double-blind trial of esketamine with a minor number of subjects. Two other trials to test efficacy fell short. Six participants died during clinical studies, three by suicide, compared to no suicides in the control group.[13]

Esketamine has serious risks because of its molecular similarity to ketamine, a “club” and “date rape” drug—also prescribed to treat depression without FDA approval.
Esketamine has serious risks because of its molecular similarity to ketamine, a “club” and “date rape” drug—also prescribed to treat depression without FDA approval.[14] It carries a prominent warning: “Patients are at risk for dissociative or perceptual changes after administration” and it has the potential, like ketamine, to be abused.[15]
Since 1992, reports about propofol have been published (largely in forensic medical journals) concerning the drug’s abuse, accidental overdose and suicide associated with it. At least 38 human cases of abuse/dependency were published in peer-reviewed literature for the 15-year period from 1992 to 2007.[16]
According to a review of propofol deaths published in the Journal of the Louisiana State Medical Society, “Propofol is a dangerous drug with an evident abuse potential which often results in fatalities.”[17] Yet now it is being considered for the treatment of depression!
Other side effects include confusion, agitation, anxiety, abnormally low blood pressure, slow heartbeat and short periods of not breathing.[18] It may also cause abnormal heart electrical signals, seizures, blood clots, acute liver failure and heart failure.[19]
The principal researcher using propofol also delivers electroshock, despite admitting that with ECT, “people are going to have some degree of memory problems.”[20]
The FDA relies upon studies to approve a drug but therein lies a key problem.
- In 2016, the FDA fast tracked a drug for hallucinations and delusions associated with Parkinson’s disease and as of March 2018, there had been 887 deaths linked to it.[21]
- FDA-approved atypical (new) antipsychotics that have been linked to 15,000 deaths in nursing homes, according to congressional testimony.[22] The drugs can also cause the elderly to suffer from increased risk of strokes and death. [23] A study published in New England Journal of Medicine found the rate of sudden cardiac death doubled for those taking atypical antipsychotics and there were three such deaths per year for every 1,000 patients taking them.[24] Additionally, according to one study, antidepressants were estimated to cause 10 to 44 deaths out of 1,000 people over a year. [25] Yet the FDA has approved the use of certain antipsychotics to be used as an adjunct to antidepressants—combining two potentially lethal drugs.[26]
Claims that ECT or antidepressants re-wire dysfunctional brains and have no permanent damage or risks are reported as ‘fact,’ without any scientific evidence to confirm this. This misleads consumers into thinking ‘brain stimulation’ and drugs are correcting something ‘wrong’ in the brain when, in fact, these practices are damaging it.
CCHR urges consumers to be better informed of psychiatric treatments offered them, warning they are often nothing more than a physical and mental health assault—a terrible betrayal for people seeking help.
For more information on the adverse effects of psychiatric drugs, click here and sign CCHR’s Petition to Ban ECT here.
References:
[1] Brian Mickey et al. “Propofol for Treatment-Resistant Depression: A Pilot Study,” Int J Neuropsychopharmacol. 2018 Dec; 21(12): 1079–1089, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6276046/
[2] Ibid.
[3] https://abcnews.go.com/US/conrad-murray-michael-jackson-gave-lethal-drug-dose/story?id=21002293
[4] Op. cit., Brian Mickey et al.
[5] “‘Michael Jackson drug’ still prompts curiosity from patients,” KTXS 12 ABC News, 22 June 2019, https://ktxs.com/news/nation-world/michael-jackson-drug-still-prompts-curiosity-from-patients
[6] Ibid.
[7] Aisha Dow, “Grandfather forced to undergo ECT before ‘preventable’ death,” The Age, 18 Apr. 2018, https://www.theage.com.au/national/victoria/grandfather-forced-to-undergo-ect-before-preventable-death-20180418-p4zacy.html
[8] Dominic Gilbert, “Mental health service failure,” Eastern Daily Press, 18 Apr. 2018, https://www.edp24.co.uk/news/mental-health-failures-katherine-rought-rought-1-5480329
[9] John Read and Chelsea Arnold, “Is Electroconvulsive Therapy for Depression More Effective Than Placebo? A Systematic Review of Studies Since 2009,” Ethical Human Psychology and Psychiatry, Volume 19, Number 1, 2017, http://www.ingentaconnect.com/content/springer/ehpp/2017/00000019/00000001/art00002
[10] “HEALTH ALERT: ‘Rare but serious’ risk of suicide for patients on antidepressants, new findings reveal,” The Sun (UK), 25 June 2019, https://www.thesun.co.uk/news/9367136/antidepressants-rare-serious-risk-suicide/
[11] Allen J. Frances, M.D., “What to Do When Treatment Doesn’t Work,” Psychology Today, 29 Jul. 2016, https://www.psychologytoday.com/us/blog/saving-normal/201607/what-do-when-treatment-doesnt-work
[12] https://www.bloomberg.com/opinion/articles/2019-06-13/trump-offer-to-negotiate-j-j-depression-drug-for-vets-is-all-show
[13] “FDA Overlooked Red Flags In Drugmaker’s Testing of New Depression Medicine,” Kaiser Health News, 11 June 2019, https://khn.org/news/fdas-approval-of-new-depression-drug-overlooked-red-flags-in-its-testing/
[14] https://www.medicalnewstoday.com/articles/320409.php; https://www.psycom.net/ketamine-depression
[15] https://www.rxlist.com/spravato-drug.htm
[16] https://journals.lww.com/anesthesia-analgesia/fulltext/2009/04000/Death_from_Propofol__Accident,_Suicide,_or_Murder_.24.aspx
[17] Diaz JH, Kaye AD, “Death by Propofol,” J La State Med Soc. 2017 Mar-Apr; 169(2):28-32. Epub 2017 Apr 15, https://www.ncbi.nlm.nih.gov/pubmed/28414657
[18] https://www.rxlist.com/diprivan-side-effects-drug-center.htm
[19] https://www.webmd.com/drugs/2/drug-3519/propofol-intravenous/details/list-sideeffects
[20] “Patient seek ‘last resort’ alternatives to treat depression,” KSL Newsradio, 25 Sept. 2018.
[21] Caroline Chen, “FDA Repays Industry by Rushing Risky Drugs to Market,” Propublica, 26 June 2018, https://www.propublica.org/article/fda-repays-industry-by-rushing-risky-drugs-to-market
[22] Martha Rosenberg, “The Most Popular Drug in America Is an Antipsychotic and No One Really Knows How It Works,” Alternet, 13 Nov 2014, http://www.alternet.org/most-popular-drug-america-antipsychotic-and-no-one-really-knows-how-it-works; http://www.lifeextension.com/magazine/2012/10/the-fda-exposed-an-interview-with-dr-david-graham/page-01 David Graham’s testimony was before Congress in November 2004.
[23] Philip S. Wang, M.D., Dr. P.H., et al., “Risk of Death in Elderly Users of Conventional vs. Atypical Antipsychotic Medications,” New England Journal of Medicine, 1 Dec. 2004, 353;22.
[24] “DoD cracks down on off-label drug use,” Military Times, 29 Mar. 2013, https://www.militarytimes.com/2013/03/29/dod-cracks-down-on-off-label-drug-use/
[25] Paul Andrews, “Things Your Doctor Should Tell You About Antidepressants,” Mad in America: Science, Psychiatry and Community, 12 Sept. 2012, http://www.madinamerica.com/2012/09/things-your-doctor-should-tell-you-about-antidepressants/; https://www.psychiatrictimes.com/major-depressive-disorder/evidence-grows-value-antipsychotics-antidepressant-adjuncts



SHARE YOUR STORY/COMMENT