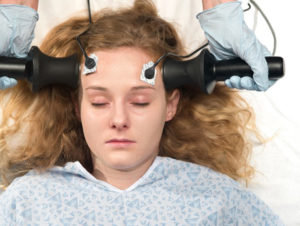
New Research Supports Electroshock Causes Brain Damage: Ban Re-urged
CCHR says new UK research on electroshock “therapy” damage—given each year to 100,000 Americans, including children as young as five—should prompt review of U.S. studies…


CCHR says new UK research on electroshock “therapy” damage—given each year to 100,000 Americans, including children as young as five—should prompt review of U.S. studies…
Here in the States, where pharmaceuticals are advertised in newspapers and magazines, radio, and especially TV, anyone seeing happy actors proclaiming how and an anti-depressant changed their lives can almost demand that drug from even a primary care physician, and usually get it.
A limited hangout is intelligence spook speak for letting out just enough information to appease investigations or grass roots suspicions. But only part of the picture is revealed, not the whole big picture…CBS did not reveal the horrible side effects from anti-depressants and psychotropic drugs. They did interview a British medical official who was part of a UK commission that banned anti-depressant use on mild to moderately depressed patients.Even Medscape lists these side effects from SSRI and SNRI anti-depressants: Abnormal bleeding, hepatitis, headache, hyponatrenia (potentially deadly low sodium), toxic epidermal necrolysis (potentially deadly skin death), impotence, abnormal sensations, mania and suicide.
We all know about the placebo effect. But a Harvard Medical School professor has applied the same theory to antidepressants and his findings are likely to rile drugmakers. Why? He filed Freedom of Information Act requests to obtain unpublished clinical trial data and found that, when combining results with published data, the various antidepressants were no better than dummy pills.
“These are the studies that show no benefit of the antidepressant over the placebo. What they did was they took more successful studies – they published most of them – and they took their unsuccessful studies, and they didn’t publish that…. If they were mildly or moderately depressed, you don’t see a difference at all. The only place where you get a clinically meaningful difference is at these very extreme levels of depression,” Irving Kirsch tells 60 Minutes.
For any mental illness or passing mood swing that may trouble a person, the Diagnostic and Statistical Manual of Mental Disorders — better known as the DSM — has a label and a code. Recurring bad dreams? That may be a Nightmare Disorder, or 307.47. Narcolepsy uses the same digits in a different order: 347.00. Fancy feather ticklers? That sounds like Fetishism, or 302.81. Then there’s the ultimate catch-all for vague sadness or uneasiness, General Anxiety Disorder, or 300.02. That’s a label almost everyone can lay claim to.Drug companies are particularly eager to win over faculty psychiatrists at prestigious academic medical centers. Called “key opinion leaders” (KOLs) by the industry, these are the people who through their writing and teaching influence how mental illness will be diagnosed and treated. They also publish much of the clinical research on drugs and, most importantly, largely determine the content of the DSM. In a sense, they are the best sales force the industry could have, and are worth every cent spent on them. Of the 170 contributors to the current version of the DSM (the DSM-IV-TR), almost all of whom would be described as KOLs, ninety-five had financial ties to drug companies, including all of the contributors to the sections on mood disorders and schizophrenia.
Is America truly stricken with widespread mental illness? Do tens of millions need mind-altering drugs? A recent flurry of media articles lead readers to a realization that Big Pharma and the “mental health” industry have deceived Americans on a grand scale.
The “New York Review of Books” two-part article by Dr. Marcia Angell, Senior Lecturer at Harvard Medical School and former Editor in Chief of The New England Journal of Medicine, summarizes it extremely well. She analyzes three books by authors Irving Kirsch, Robert Whitaker, and Daniel Carlat. Each deconstructs the apparent mental illness epidemic and theory that mental disorders stem from brain chemical imbalances which can be corrected by drugs.
Dr. Angell’s review has sparked a host of other journalists to applaud her and fuel the fire. An article in Forbes even concludes, “psychopharma is looking like an idea whose time has passed.”